Pericardial effusion, an abnormal build-up of fluid in the pericardial sac surrounding the heart, poses significant health challenges. While mild cases can often be managed with medication or careful monitoring, moderate to severe or recurrent effusions may necessitate procedural intervention to relieve pressure on the heart and prevent complications such as cardiac tamponade. Traditionally, treatment involved pericardiocentesis or open surgical drainage. However, advancements in cardiac care, particularly Minimally Invasive Cardiac Surgery (MICS), now offer effective alternatives. This article delves into pericardial effusion’s causes, symptoms, diagnosis, and treatment, with a focus on how minimally invasive techniques are revolutionizing patient care.
Understanding Pericardial Effusion
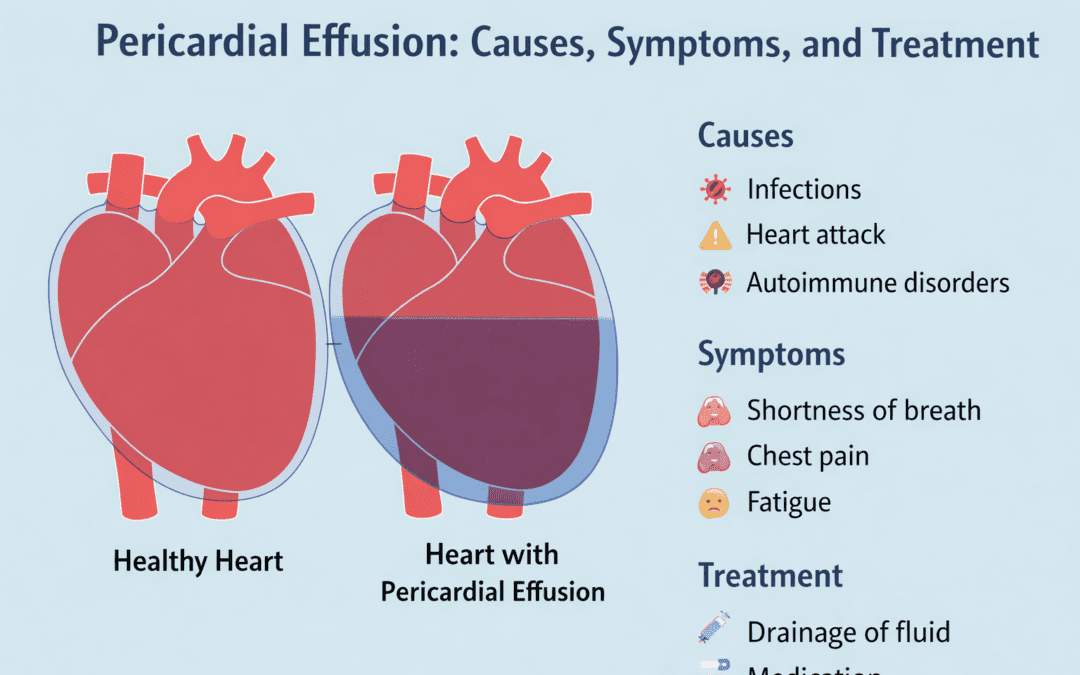
Pericardial effusion occurs when excess fluid accumulates in the pericardial cavity, the space between the heart and its surrounding sac. The pericardium typically contains a small amount of fluid to reduce friction during heartbeats. However, various conditions can lead to excessive fluid accumulation.
Common causes of pericardial effusion include infections, such as viral or bacterial pericarditis, inflammatory diseases like lupus, and trauma or injury to the chest. Cancer, hypothyroidism, and kidney failure are other potential contributors. Understanding the underlying cause is crucial for effective treatment.
Recognizing the symptoms of pericardial effusion is vital for early diagnosis. Symptoms vary depending on the severity and rate of fluid accumulation. Patients may experience chest pain, shortness of breath, fatigue, or palpitations. In severe cases, the pressure on the heart can lead to cardiac tamponade, a life-threatening condition requiring immediate intervention.
Diagnosing Pericardial Effusion
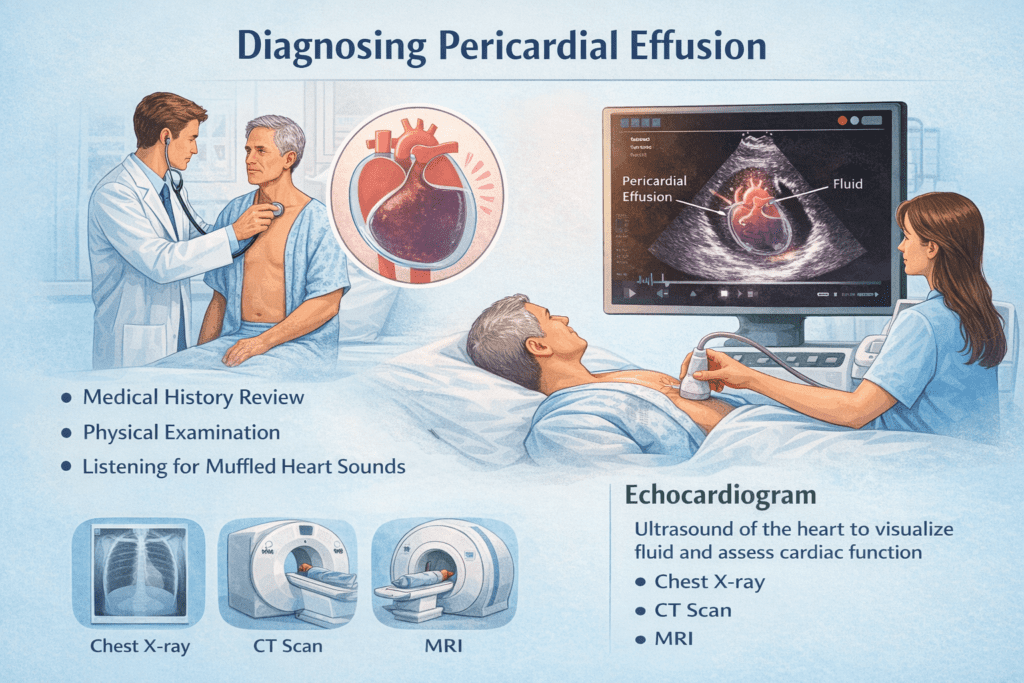
Accurate diagnosis of pericardial effusion begins with a thorough medical history and physical examination. Physicians often listen for muffled heart sounds, a hallmark of fluid accumulation. Further diagnostic tests are crucial for confirming the presence and extent of the effusion.
Echocardiography, a non-invasive ultrasound of the heart, is the primary tool for diagnosing pericardial effusion. It allows doctors to visualize the fluid around the heart and assess its impact on cardiac function. This imaging technique is vital for determining the effusion’s size and potential for tamponade.
In some cases, additional imaging tests such as chest X-rays, CT scans, or MRI may be necessary to gather more detailed information. These tests can help identify the effusion’s cause and guide treatment decisions, particularly when the underlying condition is complex or multifaceted.
Traditional Treatment Approaches
Historically, the management of pericardial effusion involved procedures like pericardiocentesis or open surgical drainage. Pericardiocentesis, a procedure where fluid is aspirated from the pericardial sac using a needle, offers immediate relief but may not address the root cause.
Open surgical drainage involves creating an incision in the chest to access and drain the fluid. While effective, this approach is invasive, requiring a longer recovery period and increased risk of complications. However, it remains a necessary option for certain complex cases.
While these methods provide relief, they often come with significant drawbacks, including the potential for infection, prolonged hospitalization, and increased healthcare costs. These challenges underscore the need for less invasive treatment options.
The Rise of Minimally Invasive Cardiac Surgery (MICS)
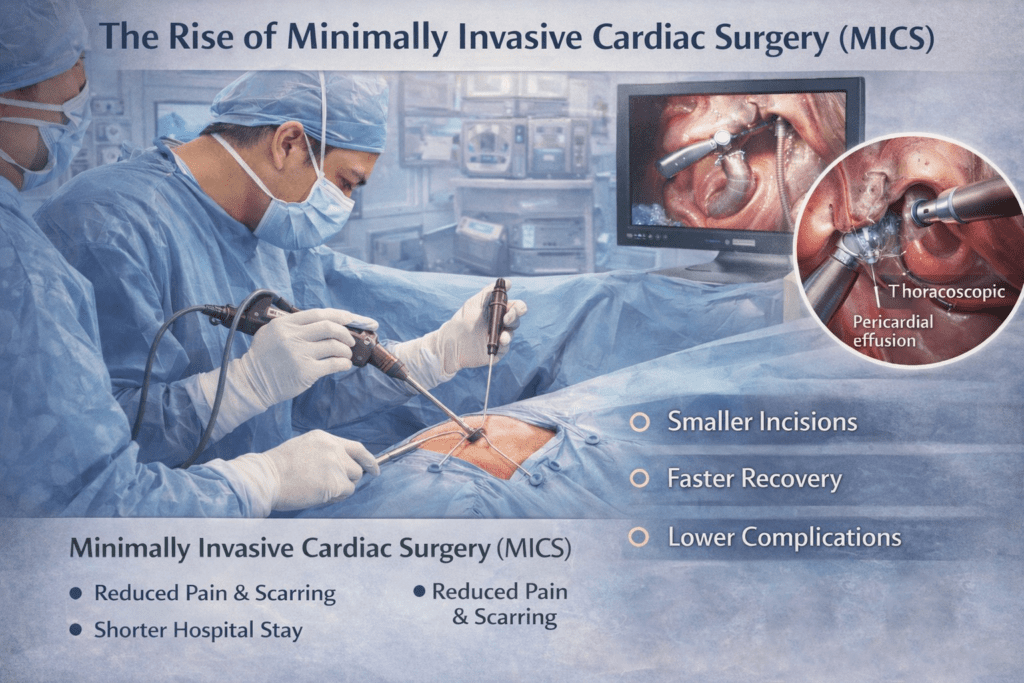
Minimally Invasive Cardiac Surgery (MICS) techniques are transforming the landscape of pericardial effusion treatment. Procedures like thoracoscopic pericardial window creation allow surgeons to drain excess fluid through small incisions, minimizing surgical trauma.
MICS offers several advantages over traditional methods. The smaller incisions result in reduced pain, shorter hospital stays, and faster recovery times. Patients often experience less scarring, contributing to improved cosmetic outcomes and overall quality of life.
Moreover, MICS techniques are associated with lower infection rates and decreased risk of complications. These benefits make minimally invasive surgery an attractive option for patients seeking effective treatment without the drawbacks of conventional open-heart surgery.
Procedure Details: Thoracoscopic Pericardial Window Creation
Thoracoscopic pericardial window creation is a key MICS technique for managing pericardial effusion. The procedure involves making small incisions in the chest, through which a camera and surgical instruments are inserted to create a drainage window in the pericardium.
This approach allows continuous drainage of fluid, preventing re-accumulation and reducing the risk of cardiac tamponade. The use of a camera provides surgeons with enhanced visualization, ensuring precision and safety during the procedure.
Patients undergoing thoracoscopic pericardial window creation typically experience minimal discomfort and can often return to normal activities within days. This rapid recovery is a significant advantage, particularly for individuals seeking to minimize disruption to their daily lives.
Benefits of Minimally Invasive Techniques
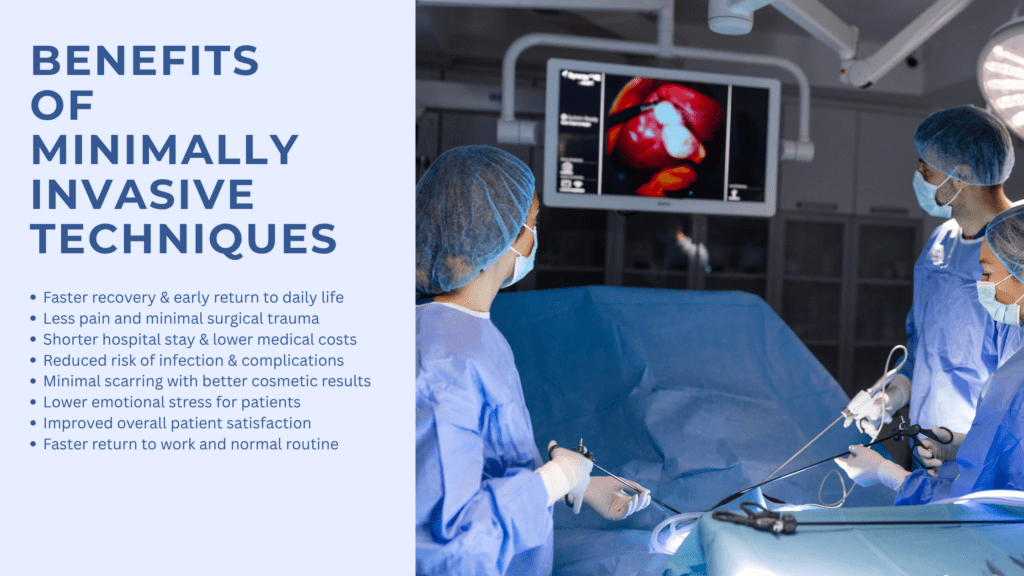
The benefits of minimally invasive techniques extend beyond immediate surgical outcomes. Patients often report higher satisfaction due to the reduced physical and emotional stress associated with smaller incisions and quicker recoveries.
From a healthcare perspective, MICS leads to cost savings by reducing hospital stays and minimizing the need for extensive postoperative care. This efficiency makes minimally invasive procedures an economically viable option for both patients and healthcare systems.
Furthermore, the reduced recovery time associated with MICS allows patients to return to their routines sooner, positively impacting their mental health and overall well-being. This holistic approach to patient care aligns with the goals of modern healthcare, emphasizing patient-centered outcomes.
Making Informed Decisions About Treatment
For patients diagnosed with pericardial effusion, understanding the available treatment options is crucial for making informed decisions. While traditional methods remain valid in certain scenarios, minimally invasive techniques offer a compelling alternative for many individuals.
Patients should engage in open discussions with their healthcare providers to assess the suitability of MICS based on their specific medical conditions and personal preferences. Factors such as the severity of the effusion, underlying health issues, and lifestyle considerations should all be taken into account.
Ultimately, the choice of treatment should be guided by a comprehensive evaluation of risks, benefits, and individual patient goals. Empowering patients with clear, evidence-based information enables them to choose the safest and most effective path to recovery.
The Future of Pericardial Effusion Treatment
As medical technology continues to evolve, minimally invasive techniques are poised to play an increasingly prominent role in the treatment of pericardial effusion. MICS offers significant advantages in terms of safety, recovery, and patient satisfaction, making it a preferred choice for many.
By focusing on reducing surgical trauma and enhancing patient outcomes, MICSHeart is committed to advancing cardiac care through innovative, patient-friendly solutions. Through continued research and development, minimally invasive techniques will likely become even more accessible and effective, further transforming heart surgery.
For patients and caregivers seeking reliable information and compassionate care, platforms like MICSHeart provide valuable resources, helping individuals navigate their treatment options with confidence and clarity. The future of cardiac surgery is here, promising a new era of safer, more efficient patient care.
Frequently Asked Questions
Q1. What are the common causes of pericardial effusion?
A1. Pericardial effusion can be caused by infections like viral or bacterial pericarditis, inflammatory diseases such as lupus, trauma, cancer, hypothyroidism, and kidney failure. Identifying the underlying cause is crucial for appropriate treatment.
Q2. How is pericardial effusion diagnosed?
A2. Diagnosis typically involves a medical history review, physical examination, and echocardiography to visualize fluid around the heart. Additional imaging tests like chest X-rays, CT scans, or MRI may be used for detailed evaluation.
Q3. What are the traditional treatments for pericardial effusion?
A3. Traditional treatments include pericardiocentesis, where fluid is aspirated using a needle, and open surgical drainage. These methods provide relief but may involve longer recovery times and higher complication risks.
Q4. What are the benefits of minimally invasive cardiac surgery for pericardial effusion?
A4. Minimally invasive techniques like thoracoscopic pericardial window creation offer reduced pain, shorter recovery times, and less scarring compared to traditional surgery. They also lower infection rates and healthcare costs.
Q5. How can patients make informed decisions about pericardial effusion treatment?
A5. Patients should discuss treatment options with healthcare providers, considering the severity of the effusion, underlying health issues, and personal preferences. Understanding the risks and benefits of each method helps in making informed choices.